What Is Kernicterus & Jaundice?

Kernicterus is a severe brain injury that can happen when jaundice in newborns is not treated appropriately.
Jaundice occurs when something in the blood called “bilirubin” accumulates. Bilirubin is a part of hemoglobin, which in turn is a part of our body’s red blood cells. The liver normally breaks down red blood cells when they die, and bilirubin is excreted in the stool as bile. When many red blood cells die at one time or if the liver’s ability to process old red blood cells is affected, too much bilirubin may build up in the blood, causing jaundice.
Because bilirubin is brownish yellow, when bilirubin levels are elevated the skin and whites of the eyes appear yellow.
If the amount of bilirubin in the blood reaches a critical level, bilirubin can enter the brain, which is what causes permanent damage. Kernicterus, i.e., brain damage, is prevented by treating jaundice early — before the bilirubin level becomes too high and crosses into the brain.
Newborns are particularly susceptible to developing jaundice. During pregnancy, a mother’s body removes extra bilirubin for the baby. After birth, it sometimes takes days for the newborn’s liver to mature enough to be efficient at removing bilirubin from the blood. Additionally, newborns create (and reabsorb from the gut) more bilirubin than adults, creating a larger bilirubin “load.” The birth process itself – for example, bruising/hematoma/hemorrhage during delivery – may injure red blood cells, releasing bilirubin. Finally, factors such as (1) blood group incompatibilities between the infant and mother and (2) infant prematurity increase the risk of jaundice.
A low-level buildup of bilirubin is normal during the first week of life and occurs in approximately 60% of babies. This is called “mild jaundice,” and it gives a newborn a slightly yellowish tint. Typically, mild jaundice resolves with feeding and time.
Inadequate feeding is an important contributor to jaundice. If an increasing bilirubin level makes a baby ill (causing poor feeding), lower intake will further increase the amount of bilirubin in the blood, making the child feel sicker — creating a dangerous cycle.
Signs of high bilirubin include a spreading, worsening yellow tint to the skin and eyes, lethargy, and excess sleeping. As the bilirubin level increases, there may be fever, a high-pitched cry, and, ultimately, decreased tone (floppiness) with episodes of increased tone and arching of the head and back.
Treatment for Jaundice
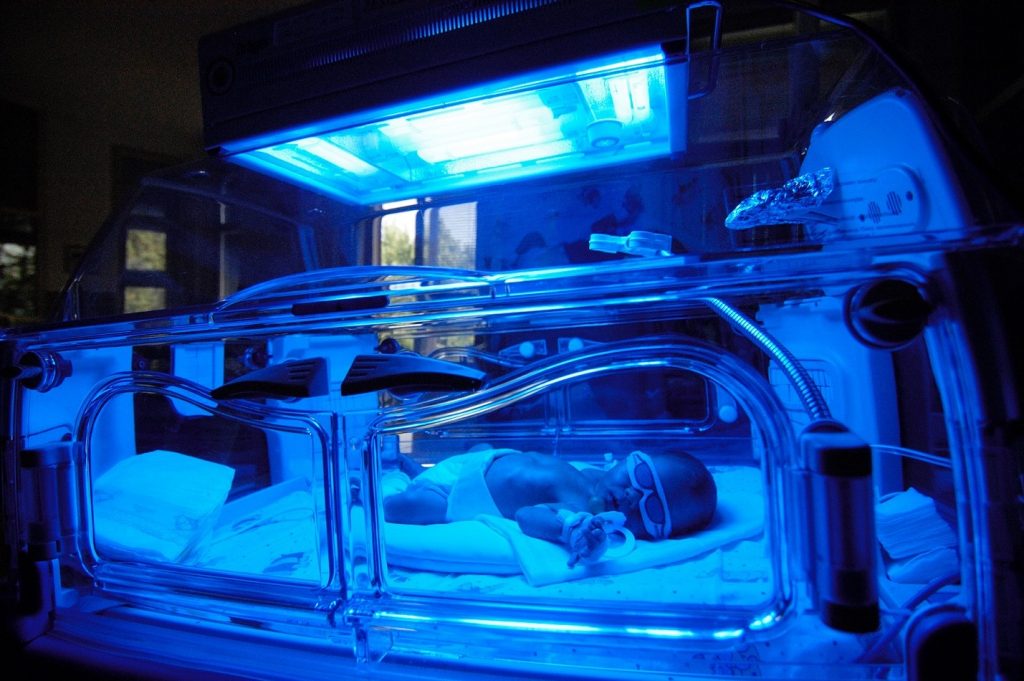
When jaundice becomes severe, doctors must take swift corrective action. Fortunately, there is effective treatment for newborns with high bilirubin levels: (1) Phototherapy (i.e., light treatment) usually is effective for a mild or moderately high bilirubin. Light, including even natural sunlight, passes through the skin and changes bilirubin into a different form that the body eliminates more easily. (2) With much higher bilirubin levels, doctors perform a blood transfusion to reduce excess bilirubin.
A very high level of bilirubin is a medical emergency.
When a baby’s bilirubin level is dangerously high, particularly with signs of kernicterus, arrangements must be made immediately for a blood transfusion. This may take a few hours, even in the best medical centers, so prompt action, as the problem is developing, is imperative. In the meantime, the baby should receive phototherapy as close as possible to the baby with maximal surface area exposed (and the eyes covered). The baby also should be fed aggressively (by tube if necessary).
Common Mistakes
When there is a serious concern about jaundice, do not let your baby’s healthcare providers make the following mistakes:
- Not measuring the bilirubin level. A bilirubin level is a very easy test to get. Preventing high bilirubin is much easier and less risky than treating it.
- Questioning a high bilirubin level and delaying treatment while testing is repeated. It is okay to repeat the test but not to delay intervention waiting for confirmation. There is nothing dangerous about treating high bilirubin, so therapy should not wait for re-testing.
- Measuring bilirubin but failing to compare it to hour-specific norms. This is very important. A bilirubin level in a one-day-old infant may be normal or dangerously high depending whether the baby is 24 or 47 hours old. A level of 8.5 would be high-risk (95th percentile) at 24 hours, but much lower risk (40th percentile) at 47 hours. Most clinicians use an algorithm (flow chart) and/or a nomogram (graph) to evaluate bilirubin levels. See figures 1 & 2 at http://pediatrics.aappublications.org/content/114/1/297.full.
- Interrupting phototherapy for diagnostic testing. Most testing can be done while the baby receives phototherapy. Even if an infant is moved, the phototherapy lights should travel with the patient.
- Not examining the baby for clinical signs of developing kernicterus.
Because jaundice is so common in babies, every pediatric/neonatal medical provider must be aware of the risks of high bilirubin and how to prevent kernicterus. There are specific national guidelines how to diagnose and manage this problem. If healthcare providers allow a baby to develop a bilirubin level of 30 mg/dL or greater it is considered so egregious that the Joint Commission (which certifies hospitals) designated it as a “sentinel event,” which should be reported. https://www.jointcommission.org/assets/1/6/20190701_2_CAMH_24_SE.pdf
Today, no child should suffer a brain injury due to kernicterus or high bilirubin. If your child has been injured by high bilirubin, it is likely that you have a strong case of medical malpractice, and that potential claim should be evaluated promptly by experienced lawyers.
The national law firm Raynes & Lawn, founded in 1970, has decades of experience representing families of children who are severely injured when hospitals and doctors fail to appropriately treat babies.
We are routinely retained by families and consulted by attorneys across the United States, having obtained large verdicts and settlements — from Maine to Florida and from California to Pennsylvania — in cases where babies suffered severe brain injuries.
We hold responsible those whose substandard behavior injures the most vulnerable patients – infants. Please visit Raynes & Lawn at https://rayneslaw.com/.
A word about statutes of limitations
Every state has a law placing a time limit on filing medical negligence claims (called a “statute of limitations”). Often that time limit is two years from the date that malpractice occurred, but some states’ rules are different. Thus, it is very important to consult an attorney quickly if you or your child may have a claim.
IMPORTANT: Most states protect the legal rights of children. Often states significantly extend the time within which one may bring a child’s claim. Even if it has been more than two years since the date of medical malpractice, in the case of an injured child, it is important to check with an attorney to determine if your state has an extended minor’s statute of limitations.
Support
Parents of Infants and Children with Kernicterus
http://pic-k.org/
References
Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics 2004;114(1):297-316, accessible at http://pediatrics.aappublications.org/content/114/1/297.full
Bhutani VK, Johnson L, Sivieri EM. Predictive ability of a predischarge hour-specific serum bilirubin for subsequent significant hyperbilirubinemia in healthy term and near-term newborns. Pediatrics 1999;103(1):6-14.
Shapiro SM. Bilirubin toxicity in the developing nervous system. Pediatric Neurology 2003;29(5):410-21.
Shapiro SM. Definition of the clinical spectrum of kernicterus and bilirubin-induced neurologic dysfunction (BIND). Journal of Perinatology 2005;25(1):54-9.
Shapiro SM, Bhutani VK, Johnson L. Hyperbilirubinemia and kernicterus. Clinics in Perinatology 2006;33(2):387-410.
Shapiro SM, Nakamura H. Bilirubin and the auditory system. Journal of Perinatology 2001;21 Suppl 1:S52-5; discussion S59-62.
