Pseudomonas Bacterial Infection and Death at the Geisinger Medical Center Neonatal Intensive Care Unit

Recently, three infants died and five others became ill from an infection at the neonatal intensive care unit (NICU) at Geisinger Medical Center in Danville, Pennsylvania. Reportedly, all of the babies were premature; and all of the babies suffered infection from the same organism: the pseudomonas bacterium.
Premature babies usually are admitted to a NICU. They are more vulnerable to infection because their immune systems are underdeveloped as a result of their prematurity. That is why it is absolutely critical that NICU staff strictly adhere to infection control measures to protect these infants.
In this case, the fact that all of these babies suffered serious infections from the same organism in the same place makes it almost certain that the exposure occurred in the Geisinger NICU. Although the pseudomonas bacterium can be found in other places, in the hospital setting it is most commonly water-borne.
Outbreaks like this are called “healthcare-associated infections (HAI),” meaning that the problem occurs in a patient as a result of care received at a health facility and was not present at the time of arrival at the facility.
In newborns, some infections can pass through the placenta to the baby. Others can transfer from the birth canal. That clearly is not what happened to these babies. Pseudomonas is not typically transmitted that way.
For many years, there have been published guidelines for NICUs establishing exactly what steps NICUs should take to protect babies from infection. The flagship journal for paediatricians is called “Pediatrics.” Paediatrics published NICU infection prevention strategies in 2012: “Strategies for Prevention of Healthcare-Associated Infections in the NICU,” Pediatrics, Vol. 129, No. 4, April 2012, pp. e1085-1093 [https://pediatrics.aappublications.org/content/129/4/e1085].
In infection cases like these, it is critical to evaluate whether the NICU staff adhered to recognized infection-prevention guidelines.
The authors of this Pediatrics paper recognized in 2012 that “. . . it is no longer acceptable to consider healthcare-associated infections as a consequence of neonatal intensive care. Rather, it is incumbent on clinicians to minimize risks of infections by performing invasive procedures only when needed and in the safest manner possible.” [Pediatrics Article at 1085 (emphasis added)]
The question in the Geisinger cases is whether the NICU staff there, in fact, took all appropriate steps to make sure that these fragile babies were protected from infection, all of their invasive procedures were necessary, and all of their procedures occurred in the “safest manner possible.”
There are several factors to look at when evaluating whether the Geisinger Medical Center NICU or any NICU is as safe as possible from this kind of infection:
Hand Washing
Most experts consider strict adherence by staff to simple hand hygiene practices to be the easiest and most effective way to reduce NICU infections. Hospitals with effective hand-hygiene practices typically have interdisciplinary quality improvement teams and recurrent training in this area; hand-washing reminders are posted in the NICU and in the staff areas. Compliance is measured and documented.
Practitioners also should use only soaps that have been validated as most effective in resisting the kinds of infections typically found in the NICU. Guidelines have been published on this subject.
Catheter-related bloodstream infections
Many premature babies require catheters. A catheter is a thin tube that can be inserted in the body to treat diseases or perform a surgical procedure. Catheters can be inserted into a body cavity, duct, or vessel. Functionally, catheters allow drainage, administration of fluids or gases, access by surgical instruments, and also perform a wide variety of other tasks.
Catheter-related bloodstream infections are the most common hospital-acquired infections in the NICU.[Pediatrics Article at 1086] This makes sense since a catheter often breaks the natural skin barrier and creates an opening for an organism to enter the body. In investigating cases such as these, catheter management is one of the first areas that must be evaluated.
Catheter equipment can look like this and includes syringes, needles, swabs, cannulas and the catheter itself:
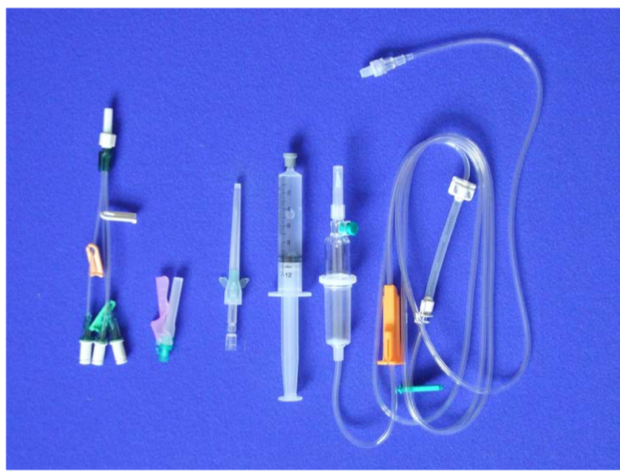
The leading causes of catheter-related infection are:
(1) Migration of skin organisms at the insertion site into the cutaneous catheter tract with the colonization of the catheter tip (usually in the first week after placement.);
(2) contamination of the catheter hub, causing colonization of long-term catheters (more common after seven days);
(3) inadvertent contamination of prepared supplies/pharmaceuticals (e.g., IV fluid, infant formula, general medications).
Only a careful review of the medical record by a physician/nurse expert can reveal the source in an individual case. Unfortunately, sometimes no obvious cause ever can be uncovered.
When evaluating the likely origin of an infection, it is critical to determine whether the NICU staff adhered to clinical practice guidelines for the insertion and maintenance of indwelling lines. Sometimes NICU personnel will leave in catheters too long. Catheter sites must be monitored on a daily basis and redressed and cleaned on a regular basis. These things should be documented.
All indwelling devices must be removed when they are no longer essential. [Pediatrics Article at 1087] In our experience, this is the single biggest problem leading to infection: Clinicians leave in catheters after they are not necessary. The longer the catheter is in place, the greater the risk of infection.
When evaluating an outbreak where many babies suffered the same infection, one can and should employ epidemiological methods to find an infection source common to all who were affected. These tools make situations like this easier to prove than an isolated infection, i.e., one baby.
Legal Issues
In any medical negligence case in Pennsylvania, the plaintiff (the person bringing the claim) must prove that the defendant hospital’s personnel were negligent. That means proving that staff failed to follow established guidelines or practices – often called “the standard of care” – or otherwise acted unreasonably. In short, it means showing that the hospital did something wrong. A bad outcome alone is not enough.
It certainly means hiring appropriately trained medical professionals, e.g., doctors and nurses, who can prove that the hospital staff acted inappropriately. It also requires proving that, if the hospital had acted appropriately, the infection would not have occurred or the baby would not have succumbed to the infection.
This is a complex and expensive process that warrants retaining a law firm with significant experience – not only in medical malpractice – but also with infection cases specifically.
In Pennsylvania, claims of medical malpractice resulting in death, with very limited exception must be brought within two years. Because these matters are complex and require a great deal of time to work up, those considering bringing such a claim should consult an experienced medical malpractice attorney as soon as possible.
When there is a pseudomonas infection in a NICU, investigators will look first at the babies’ respiratory or pulmonary care. Premature infants often receive mechanical ventilation, which involves placing a tube in a child’s trachea to help with breathing. This is the most likely place for the pseudomonas bacterium to enter the body.
Mechanical ventilation affects the body’s ability to remove mucous from the lungs and causes pooling of secretions, inflammation and even scar formation. Thus, there is significant risk of infection. Doctors, therefore, will remove endotracheal tubes as soon as possible to reduce that risk. It is very important to evaluate whether a breathing tube remained too long in every baby with such an infection. One must also review the care provided by the respiratory team, i.e., was there a breakdown in respiratory therapy technique. This usually means checking to see if staff followed protocols for changing things like ventilator tubing.
Occasionally, an outside vendor who provided supplies and materials for the respiratory equipment is the source of infection.
Investigators also must check plumbing and water supplies since pseudomonas is often waterborne.
Typically, these investigations require not only a neonatologist but also an infectious disease specialist and a microbiologist.
